Advice and guidance overview for the NHS e-Referral Service (e-RS)
Advice and guidance allows a clinician to seek advice from another. It is a communication between two clinicians: the “requesting” clinician and the provider of a service (the “responding” clinician).
What is advice and guidance and when might it be used
Advice and guidance allows one clinician to seek advice from another. Unlike creating a booking request, where a number of providers can be selected, advice and guidance is a communication between two clinicians: the “requesting” clinician and the provider of a service (the “responding” clinician).
The reasons why a clinician may wish to seek advice and guidance include:
- asking another clinician or specialist for their advice on a treatment plan and/or the ongoing management of a patient
- asking for clarification (or advice) regarding a patient’s test results
- seeking advice on the appropriateness of a referral for their patient for example, whether to refer, or what the most appropriate alternative care pathway might be
- identifying the most clinically appropriate service to refer a patient into (and how to find that service for example, what clinical term to search on
The requester is able to attach documents to the advice request, which may include diagnostic results, scanned images (for example, ECGs) or previous correspondence related to the patient. They are also able to authorise the responder to convert the request to a referral. The responder is then able to review the request (along with any attachments that may have been added) and, if required, add attachments, such as a proposed treatment plan or links to external documents and websites, before sending a response back to the requestor or converting the request into a referral, where authorisation has been given.
Below is an example image of an advice and guidance conversation.
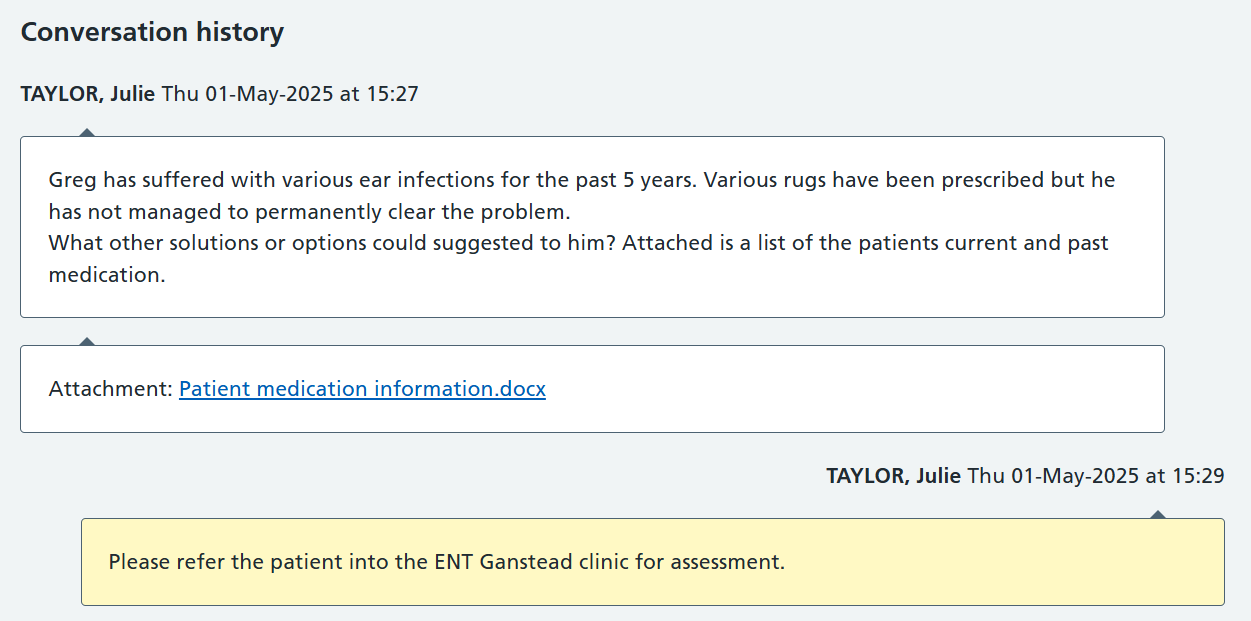
Benefits of using advice and guidance
Patient
- the patient only starts the formal referral process once appropriate advice has been received (indicating the best clinical pathway or management route) or the provider accepts to convert the request
- patients do not book an appointment that may subsequently be cancelled and redirected to another service, or rejected
- providing authorisation to convert the request to a referral may accelerate the referral process
Requesting clinician
- used as an education resource, for the clinician – this may help with future management of patients
- reduces the risk of a redirection or rejection of the referral and will better ensure that the correct services are offered to the patient
- may enable the patient to be managed in a community setting, with no need to refer to a secondary organisation
- where authorisation to convert the request to a referral is given, the provider can process this which will save time for the referrer and patient
Provider clinician
- only patients that need to be in the service are seen by the specialist – more cost-effective use of clinician time and expertise
- advice can be given regarding appropriate diagnostic tests required before an appointment is booked
- referrals can be channelled to the correct consultant (this is especially useful if named clinician referrals are enabled)
- where authorisation to convert the request to a referral is given, the provider can efficiently book the patient an appointment, in some case negating the need for further clinical review
Commissioners
- provides greater confidence that the referrals reaching secondary care are appropriate for that setting
- it helps to support GPs awareness of alternative services available within the community setting
- if a patient can be treated in another environment this may result in some savings for the commissioning organisation
Provider Organisation
- if only clinically appropriate patients are booked into a clinic there will be an ease on the demand for a service, as inappropriate patients are not taking slots that are more appropriately needed by others
- this will help the provider organisation ensure that the patient’s pathway is kept to a minimum and that delays are not introduced due to the need to redirect patients
- if the patient is booked into the right place at the right time, less administrative time is taken up ensuring that the patient is moved and seen in the correct service
- providers should be better able to manage their 18-week RTT times, as patients who are eventually referred should be better clinically prepared
- there will be a reduction in the number of patients that find themselves in the Appointment Slot Issue (ASI) process and have to be managed outside of e-RS by the provider organisation
How a service indicates that it will provide advice to requesting clinicians
When setting a service up on e-RS, a number of factors need to be considered, one of which is whether or not to offer advice and guidance. Providers must also consider any contractual requirements. For example, the Service Conditions of the 2020-2021 Standard Contract state:
6.2.3 the Provider must offer clinical advice and guidance to GPs on potential Referrals through the NHS e-Referral Service, whether this leads to a Referral being made or not.
If providers are going to offer advice through e-RS, they must consider:
Review and response process
- if clinicians are reviewing on line or through a central admin team
- how the responses will get back to the requesting clinician
- how to ensure the service can be provided consistently for example, holiday and sick leave are covered
Agreed turnaround time for response
- how quickly the requesting clinician will receive a response – agree an acceptable timeframe.
Service Definer’s role
- ensuring that the correct clinicians have access to the service and are in the correct workgroup to allow them to easily process the request
If a service is not enabled to offer advice, then, if a requester selects ’advice’ and adds search criteria (for example, Clinical Term, Speciality/Clinic Type or Named Consultant), this service will not be returned, that is only those services that have indicated they will provide advice will be displayed.
Advice and guidance and the RTT clock
If the requesting clinician is seeking advice prior to (or instead of) referring a patient, then this has no impact on the commencement of the patient’s clock start.
The RTT clock start date is the date that the provider converts the request or receives notice of the referral. For e-RS referrals this is the earliest date that a patient converts (books) their Unique Booking Reference Number or enters the ‘Defer to Provider’ (Appointment Slot Issue) process.
Is there a tariff for advice and guidance
There is no national tariff to provide advice and guidance. It is already covered within the service conditions of the NHS standard contract.
In some local health communities, providers and ICBs have agreed a nominal tariff for advice and guidance, to cover some of the administrative costs in setting up such a service. This is anticipated to be recouped by reducing the number of patients who are being referred and managed within a secondary care setting. It is also recognised that this is likely to be far less expensive than setting up administrative referral management centres, which often add no clinical benefit for patients and can be very unpopular with doctors.
Support information
Further resources including videos can be found at the support information page
Last edited: 11 June 2025 4:19 pm